Treat the person, not the disease: Treating “conditions” leads to duplicate treatments, higher costs
02/08/2019 / By Jhoanna Robinson
Strategies currently employed for treating patients with a myriad of chronic diseases are financially burdening their country’s health systems and individuals unnecessarily, a global study initiated by the National University of Singapore and the University of Melbourne in Australia has revealed. According to experts, the current clinical practice of handling each disease in isolation can result in unnecessary, duplicitive prescriptions.
The research team studied raw data from 14 global studies that took into consideration the out-of-pocket expenditure – costs not covered by insurance – of patients with multiple chronic diseases. These patients, who have what is characterized as multi-morbidity, take on the burden of high out-of-pocket costs, leading them to possibly stop taking their medication in the long run. The elderly and low-income groups are the most vulnerable.
“Patients may have financial support from insurance benefits to visit their general practitioners or go for medical checkups, but the weakest link is the lack of financial support to pay for any medications prescribed. Our research also found a common coping mechanism by some patients with high spending on medicines is non-adherence, whereby patients stop taking their medicines by failing to refill their prescriptions, which is a substantial healthcare issue,” said Dr. Grace Sum Chi-En, lead author from the National University of Singapore.
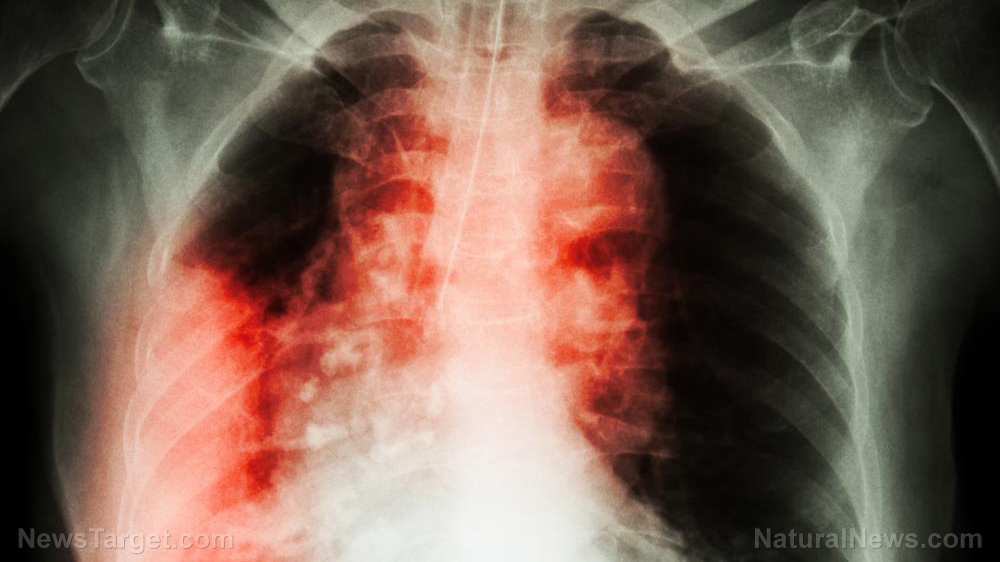
Dr. Chi-En noted that chronic diseases are not infectious and are, for the most part, long-term, which include arthritis, cancer, depression, diabetes, hypertension, obesity, and stroke. (Related: Diets lacking fresh, whole foods lead to multiple chronic diseases, study confirms.)
Researchers have noted that the yearly out-of-pocket expenditure has grown by an average of 2.7 times.
“The nature of chronic diseases is that they require long-term management and usually cannot be cured, which exacerbates the high cost to patients for medicines over a long period of time. It is imperative for healthcare policymakers to start recognizing this problem, in order to design better policies that offer financial protection on medicines for chronic diseases,” Dr. Chi-En said.
For his part, Dr. John Tayu Lee, senior author from the Nossal Institute of Global Health at the University of Melbourne, said: “Despite multi-morbidity being the norm rather than the exception for the older population, current clinical practice remains focused on single chronic disease in isolation. Our findings suggest that we need to think more carefully about how to improve the cost-effectiveness of treating patients with multiple chronic diseases.”
More on multimorbidity
Mutimorbidity is an issue that should be focused on in healthcare because it is linked to polypharmacy and higher rates of adverse drug events, reduced quality of life, higher mortality rates, and the high use of unplanned health care. Patients with multi-morbidity may be handled by both primary care and multiple specialists, who are possibly not communicating with each other regarding a particular patient’s condition.
For more stories and studies on prescription drugs and other medications, visit Opioids.news.
Sources include:
Tagged Under: Big Pharma, chronic diseases, disease causes, disease suppression, duplicate treatments, health care, multimorbidity, nutrient deficiency, Prescription drugs, senior care